Built for revenue cycle & billing leaders
When documentation, authorizations, and facility billing stay in sync, month-end stops being a fire drill. Phoenix connects clinical work to claims, AR, and reporting in one platform.
- ·Close-out checklists for unsigned docs, CPT, minutes, auths, LCD, and discharge — including batch close-outs across facilities.
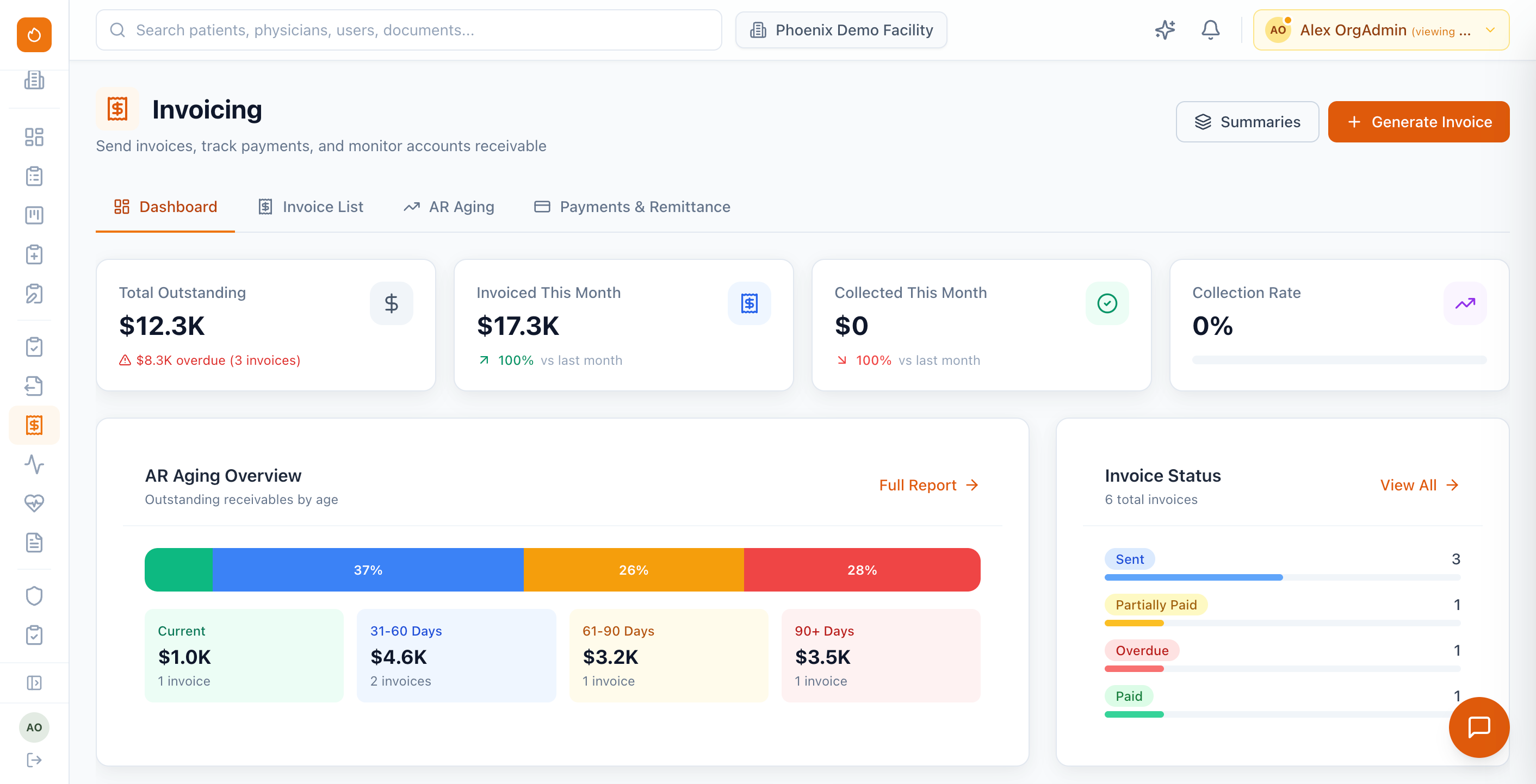
- ·Claims & remits: UB-04, CMS-1500, 837, ERA/payment import, AR aging, denials, and statements.
- ·RCM front door: referrals, verification, prior auth, onboarding, plus a patient portal for intake and consents.
- ·Authorizations enforced in scheduling and billing, with a managed care hub for caps and utilization.
- ·50+ reports, custom builder, AI dashboards, and exports to Excel or PDF — plus PDF packets for audits.
Capture every referral,
close every loop
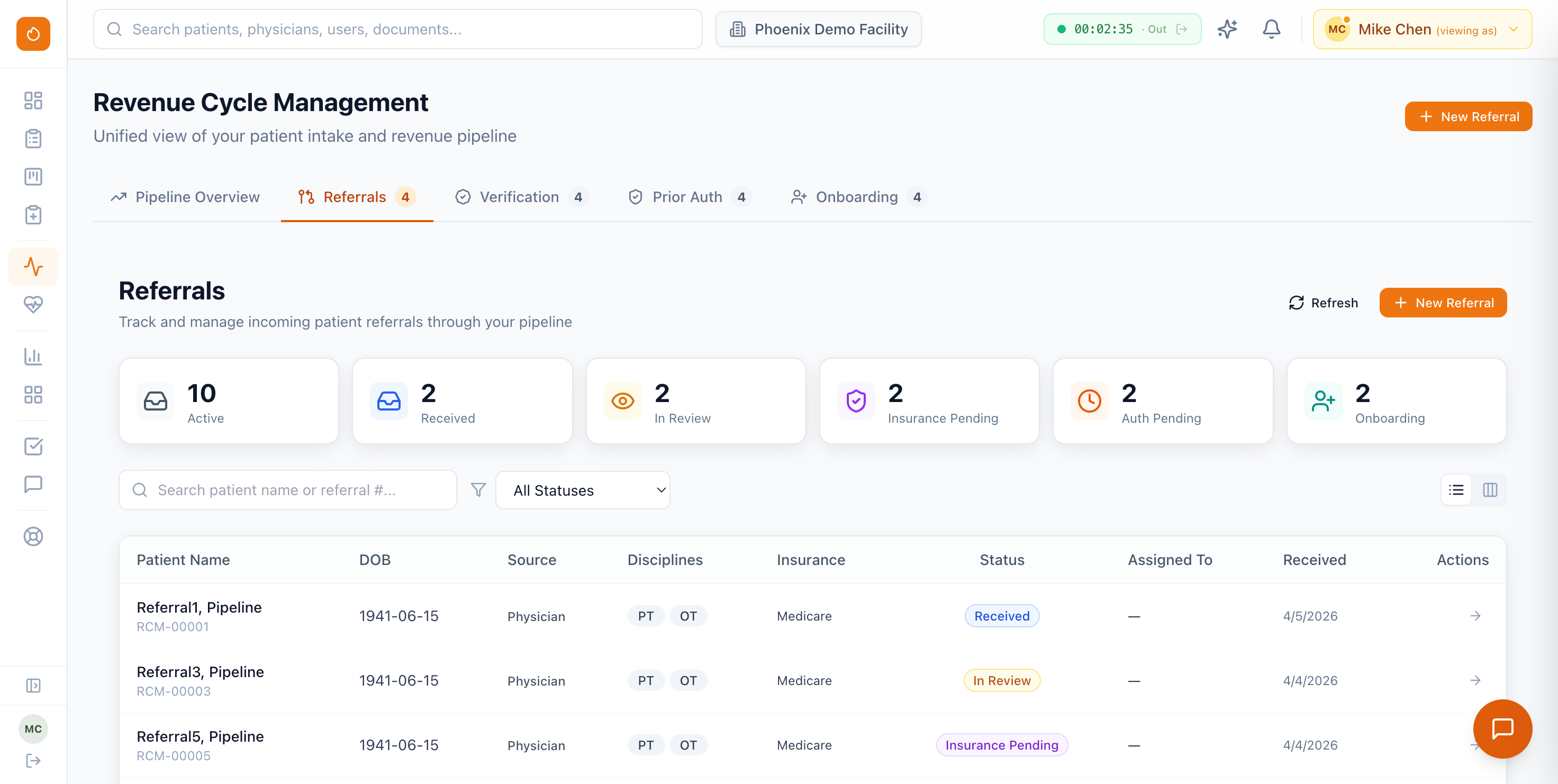
From the moment a referral hits your desk to the patient's first appointment, Phoenix Therapy tracks the entire revenue cycle pipeline — so nothing gets lost and no revenue slips through the cracks.
Capture referrals from any source with structured intake forms. Track status, assigned therapist, and facility across every referral in your pipeline.
Verify patient coverage and benefits before the first visit. Flag payor-specific requirements, copays, and deductibles up front.
Submit and track prior auth requests with approved CPT codes, visit limits, and expiration dates. Alerts fire before auths run out.
Send patients a digital intake link to complete forms, consent documents, and demographic information before their first visit — reducing front-desk bottlenecks.
Track managed care contracts, authorization utilization, visit caps, and minute limits — with alerts when patients approach or exceed authorized levels.
Close the month
with confidence
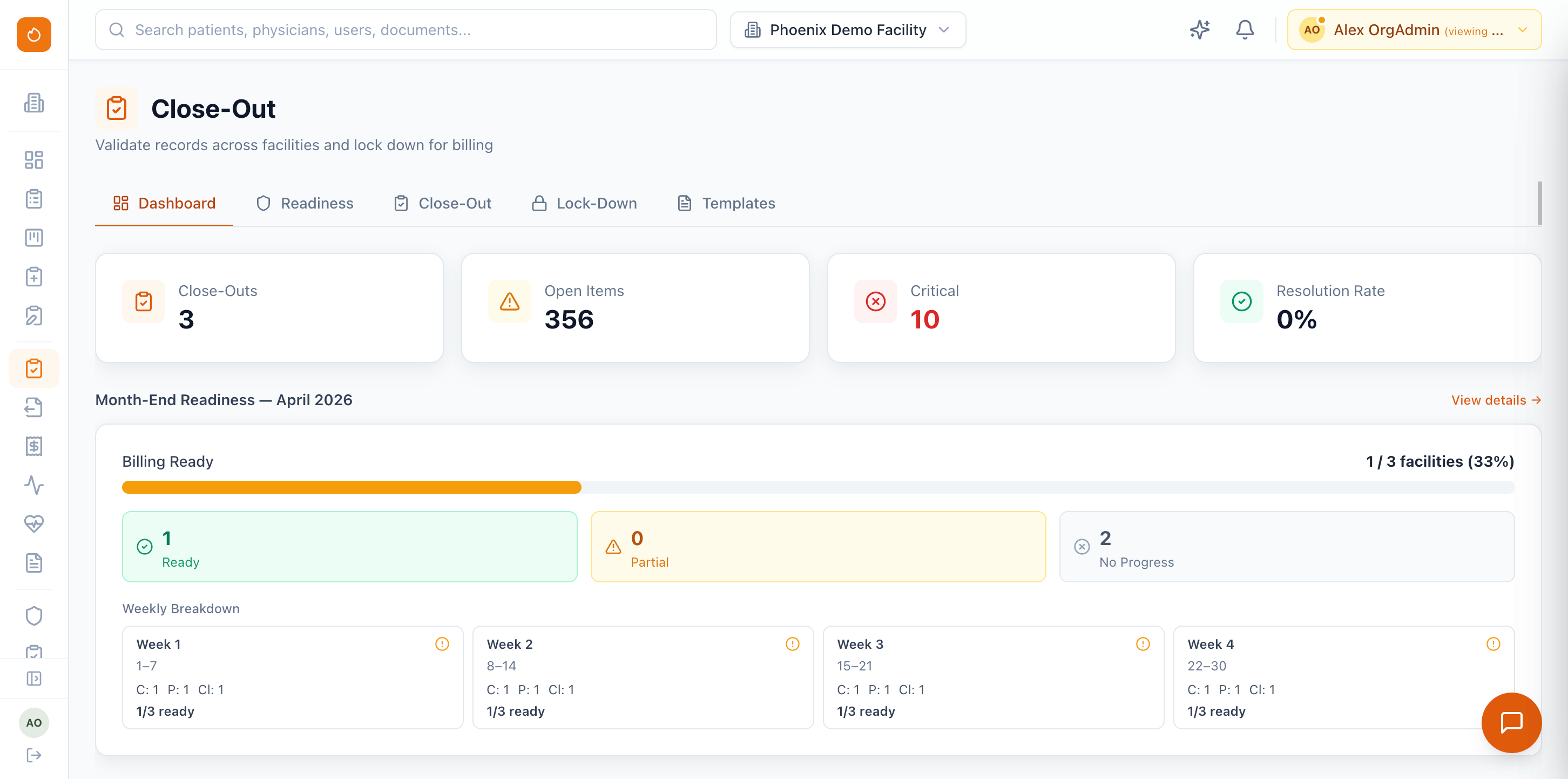
No more scrambling at month-end. Phoenix Therapy's billing engine handles everything from close-out checklists and claims generation through payment posting and AR management — across every payor and contract model.
Run batch close-outs across multiple facilities at once. Assemble billing packets with invoices, service logs, UB-04s, and biller CSVs — ready for payor submission.
Generate UB-04, CMS-1500, and X12 837I/P electronic claims directly from validated invoices. Export EMR data, biller CSVs, and custom file formats for any clearinghouse.
Configurable billing edit rules catch errors before export — CPT validation, LCD compliance, minutes reconciliation, expired authorizations, and unsigned documents in a single pre-billing check.
Import payment files and ERA remittances, match to invoices, and track payment status. Statement generation (monthly, past-due, final) and denial tracking are built in.
Full AR aging with 0–30, 31–60, 61–90, 91–120, and 120+ day buckets. Top payors by outstanding balance, collection rate tracking, days-in-AR trends, and denial analysis in one dashboard.
Manage therapy contracts with flexible billing models — CMG/HIPPS, CPT-based, per-minute, per-visit, per-unit, and Medicare fee schedule — with caps, special rates, and excluded codes.
Generate invoices, track payments, manage voids, and monitor outstanding AR — all inside the platform with full audit history.
Billing data flows
to and from the facility EHR
Native PointClickCare and MatrixCare integrations keep the right clinical and billing context in sync — PCC: therapy tab, patient ADT/census (admit, discharge, transfer), MDS (Minimum Data Set) sync, Section GG (functional status for PDPM), billing and charges, and clinical documents; MatrixCare: patient ADT/census (admit, discharge, transfer), occurrence codes (billing context), diagnosis codes (ICD-10), Section O (MDS therapy items), billing and charges, and clinical documents — so your billing team spends less time reconciling across systems.
PCC: therapy tab, patient ADT/census (admit, discharge, transfer), MDS (Minimum Data Set) sync, Section GG (functional status for PDPM), billing and charges, clinical documents. MatrixCare: patient ADT/census (admit, discharge, transfer), occurrence codes (billing context), diagnosis codes (ICD-10), Section O (MDS therapy items), billing and charges, clinical documents.
New admissions, discharges, and room transfers flow from the facility EHR into Phoenix in real time — no manual census updates needed.
Map facility-level payor plans to your billing configurations. Insurance data, plan codes, and billing identifiers stay consistent between systems.
Customer-facing REST API and FHIR R4 endpoints for custom integrations with clearinghouses, practice management systems, and other third-party platforms.
Walk through close-out with your metrics
We’ll connect documentation, auths, and billing workflows to how your team actually finishes the month.
Request a demo